Appealing trials utilizing crafted antibodies recommend that “practical treatments” might remain in reach.
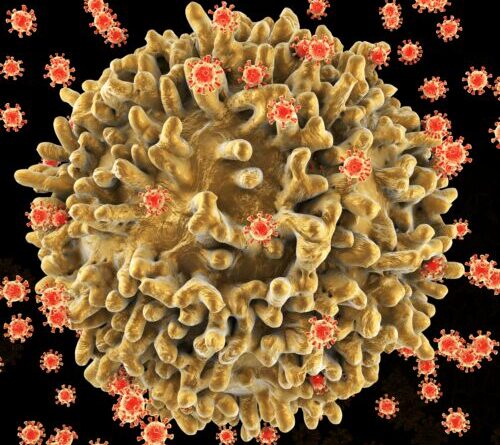
A digital illustration of an HIV-infected T cell. As soon as contaminated, the immune cell is pirated by the infection to produce and launch lots of brand-new viral particles before passing away. As more T-cells are ruined, the body immune system is gradually compromised.
Credit: Kateryna Kon/Science Photo Library by means of Getty Images
Worldwide, some 40 million individuals are dealing with HIV. And though development in treatment implies the infection isn’t the death sentence it as soon as was, scientists have actually never ever had the ability to produce a remedy. Rather, HIV-positive individuals should take a mixed drink of antiretroviral drugs for the rest of their lives.
In 2025, scientists reported a development that recommends that a “practical” treatment for HIV– a method to keep HIV under control long-lasting without consistent treatment– might certainly be possible. In 2 independent trials utilizing infusions of crafted antibodies, some individuals stayed healthy without taking antiretrovirals, long after the interventions ended.
In among the trials– the FRESH trial, led by virologist Thumbi Ndung’u of the University of KwaZulu-Natal and the Africa Health Research Institute in South Africa– 4 of 20 individuals preserved undetected levels of HIV for a mean of 1.5 years without taking antiretrovirals. In the other, the RIO trial embeded in the United Kingdom and Denmark and led by Sarah Fidler, a medical professional and HIV research study professional at Imperial College London, 6 of 34 HIV-positive individuals have actually kept viral control for a minimum of 2 years.
These landmark proof-of-concept trials reveal that the body immune system can be utilized to combat HIV. Scientists are now wanting to perform bigger, more representative trials to see whether antibodies can be enhanced to work for more individuals.
“I do believe that this sort of treatment has the chance to truly move the dial,” Fidler states, “since they are long-acting drugs”– with impacts that can continue even after they’re no longer in the body. “So far, we have not seen anything that works like that.”
Individuals with HIV can live long, healthy lives if they take antiretrovirals. Their life expectancies are still normally much shorter than those of individuals without the infection. And for lots of, everyday tablets or perhaps the more recent, bimonthly injections present substantial monetary, useful, and social difficulties, consisting of preconception. “Probably for the last about 15 or 20 years, there’s been this genuine push to go, ‘How can we do much better?'” states Fidler.
The dream, she states, is “what individuals call treating HIV, or a remission in HIV.” That has actually provided a big obstacle since HIV is a master of camouflage. The infection progresses so rapidly after infection that the body can’t produce brand-new antibodies rapidly enough to acknowledge and neutralize it.
And some HIV hides in cells in a non-active state, unnoticeable to the body immune system. These evasion techniques have actually outsmarted a long succession of treatment efforts. Aside from a handful of remarkable stem-cell transplants, interventions have actually regularly disappointed a total treatment– one that completely clears HIV from the body.
A practical treatment would be the next finest thing. Which’s where an unusual phenomenon provides hope: Some people with long-lasting HIV do ultimately produce antibodies that can reduce the effects of the infection, though far too late to completely shake it. These powerful antibodies target important, hardly ever altering parts of HIV proteins in the external viral membrane; these proteins are utilized by the infection to contaminate cells. The antibodies, able to acknowledge a broad series of infection pressures, are described broadly reducing the effects of.
Researchers are now racing to discover the most powerful broadly reducing the effects of antibodies and engineer them into a practical treatment. FRESH and RIO are perhaps the most appealing efforts.
In the FRESH trial, researchers selected 2 antibodies that, integrated, were most likely to be efficient versus HIV pressures referred to as HIV-1 clade C, which is dominant in sub-Saharan Africa. The trial registered girls from a high-prevalence neighborhood as part of a more comprehensive social empowerment program. The program had actually begun the females on HIV treatment within 3 days of their infection numerous years previously.
The RIO trial, on the other hand, picked 2 well-studied antibodies revealed to be broadly efficient. Its individuals were mainly white males around age 40 who likewise had actually gone on antiretroviral drugs not long after infection. The majority of had HIV-1 clade B, which is more common in Europe.
By matching antibodies, the scientists intended to reduce the probability that HIV would establish resistance– a typical obstacle in antibody treatments– considering that the infection would require several anomalies to avert both.
Individuals in both trials were provided an injection of the antibodies, which were customized to last around 6 months in the body. Their treatment with antiviral medications was stopped briefly. The hope was that the antibodies would deal with the body immune system to eliminate active HIV particles, keeping the infection in check. If the result didn’t last, HIV levels would increase after the antibodies had actually been broken down, and the individuals would resume antiretroviral treatment.
Excitingly, nevertheless, findings in both trials recommended that, in some individuals, the interventions triggered a continuous, independent immune action, which scientists compared to the result of a vaccine.
In the RIO trial, 22 of the 34 individuals getting broadly reducing the effects of antibodies had actually not experienced a viral rebound by 20 weeks. At this moment, they were provided another antibody shot. Beyond 96 weeks– long after the antibodies had actually vanished– 6 still had viral levels low enough to stay off antiviral medications.
An extra 34 individuals consisted of in the research study as controls got just a saline infusion and primarily needed to resume treatment in 4 to 6 weeks; all however 3 were back on treatment within 20 weeks.
A comparable pattern was observed in FRESH (although, due to the fact that it was primarily a security research study, this trial did not consist of control individuals). 6 of the 20 individuals maintained viral suppression for 48 weeks after the antibody infusion, and of those, 4 stayed off treatment for more than a year. 2 and a half years after the intervention, one stays off antiretroviral medication. 2 others likewise preserved viral control however ultimately picked to go back on treatment for individual and logistical factors.
It’s unidentified when the infection may rebound, so the scientists beware about calling individuals in remission functionally treated. The antibodies plainly appear to coax the immune system to combat the infection. Connected to contaminated cells, they indicate to immune cells to come in and eliminate.
And significantly, scientists think that this immune action to the antibodies might likewise promote immune cells called CD8+ T cells, which then pursue HIV-infected cells. This might develop an “immune memory” that assists the body control HIV even after the antibodies are gone.
The reaction looks like the immune control seen in a small group (less than 1 percent) of people with HIV, called elite controllers. These people reduce HIV without the aid of antiretrovirals, restricting it mainly to little tanks. That the trials assisted some individuals do something comparable is interesting, states Joel Blankson, a contagious illness professional at Johns Hopkins Medicine, who coauthored a short article about natural HIV controllers in the 2024 Annual Review of Immunology. “It may teach us how to be able to do this much better, and we may be able to get a greater portion of individuals in remission.”
Something researchers do understand is that the probability of accomplishing continual control is greater if individuals begin antiretroviral treatment not long after infection, when their body immune systems are still undamaged and their viral tanks are little.
Post-treatment control can take place even in individuals who began taking antiretrovirals a long time after they were at first contaminated: a group understood as chronically contaminated clients. “It simply takes place less typically,” Blankson states. “So it’s possible the methods that are associated with these research studies will likewise use to clients who are chronically contaminated.”
An especially appealing finding of the RIO trial was that the antibodies likewise impacted inactive HIV hiding in some cells. These tanks are how the infection rebounds when individuals stop treatment, and antibodies aren’t believed to touch them. Scientist hypothesize that the T cells enhanced by the antibodies can acknowledge and eliminate latently contaminated cells that show even trace quantities of HIV on their surface area.
The FRESH intervention, on the other hand, targeted the persistent HIV tanks more straight through integrating another drug, called vesatolimod. It’s created to promote immune cells to react to the HIV danger, and ideally to “shock” inactive HIV particles out of hiding. As soon as that takes place, the body immune system, with the assistance of the antibodies, can acknowledge and eliminate them.
The outcomes of FRESH are amazing, Ndung’u states, “due to the fact that it may show that this routine worked, to a level. Since this was a little research study, it’s hard to, certainly, make really difficult conclusions.” His group is still examining the information.
As soon as he protects financing, Ndung’u intends to run a bigger South Africa-based trial consisting of chronically contaminated people. Fidler’s group, on the other hand, is hiring for a 3rd arm of RIO to attempt to figure out whether stopping briefly antiretroviral treatment for longer before administering the antibodies triggers a more powerful immune reaction.
An associated UK-based trial, called AbVax, will include a T-cell-stimulating drug to the mix to see whether it boosts the lasting, vaccine-like impact of the antibodies. “It might be that integrating various methods improves various littles the body immune system, which’s the method forward,” states Fidler, who is a co-principal private investigator on that research study.
In the meantime, Fidler and Ndung’u will continue to track the virally reduced individuals– who, for the very first time considering that they got their HIV medical diagnoses, are living devoid of the needs of everyday treatment.
This story initially appeared at Knowable Magazine.
Knowable Magazine checks out the real-world significance of academic resolve a journalistic lens.
42 Comments
Find out more
As an Amazon Associate I earn from qualifying purchases.